|
Now is the time to make sure your network is ready for a hybrid world where the workplace is anywhere, endpoints could be anything, and applications are hosted all over the place. Extending the power of the secure network as close to the edge as possible helps you to better respond to the unexpected… transforming the challenges of hybrid work into opportunities for innovation. Introducing Cisco® Catalyst® 9200CX compact switchesAs part of the Catalyst 9000 family, these highly anticipated compact switches bring IOS® XE and enterprise-class access down to the very edge with an extra level of security, and the features required to handle our ever-changing world of hybrid work. The new compact Catalyst 9200CX models are optimized for flexibility and security and are ideal for
The smaller footprint and quiet, fan-less design means Catalyst 9200CX compact switches can go in places other switches cannot, like on or under a desk, mounted on the wall or ceiling, or in a closet, hospital room, or classroom. But at the same time, they offer many advanced features that are firsts for a compact switch:
And to top it off, they’re also IPsec, AVB/PTP, and BGP EVPN hardware ready. The Catalyst 9200CX is designed to allow you to secure your network from the inside out, applying continuous zero-trust security anywhere you need it, and often extending your network to places it has never been before. Whether in the board room or the bedroom, at the checkout counter, or the check-in desk, don’t box in your network to a traditional workspace or workplace; embrace the future of hybrid work with Catalyst 9200CX compact switches. ”We are excited about the new Catalyst 9200CX compact switch, which suits our needs in our Fiber to the Edge deployment at our new hospital, with advanced features such as VxLAN, VRFs and BGP.” Michael Valeur, Business Development Manager, Infrastructure, University Hospital, Region South, Denmark
Additional Resources: https://www.cisco.com/c/en/us/products/switches/catalyst-9200-series-switches/index.html from https://ift.tt/VYJQoNt Check out http://felpec.wordpress.com
0 Comments
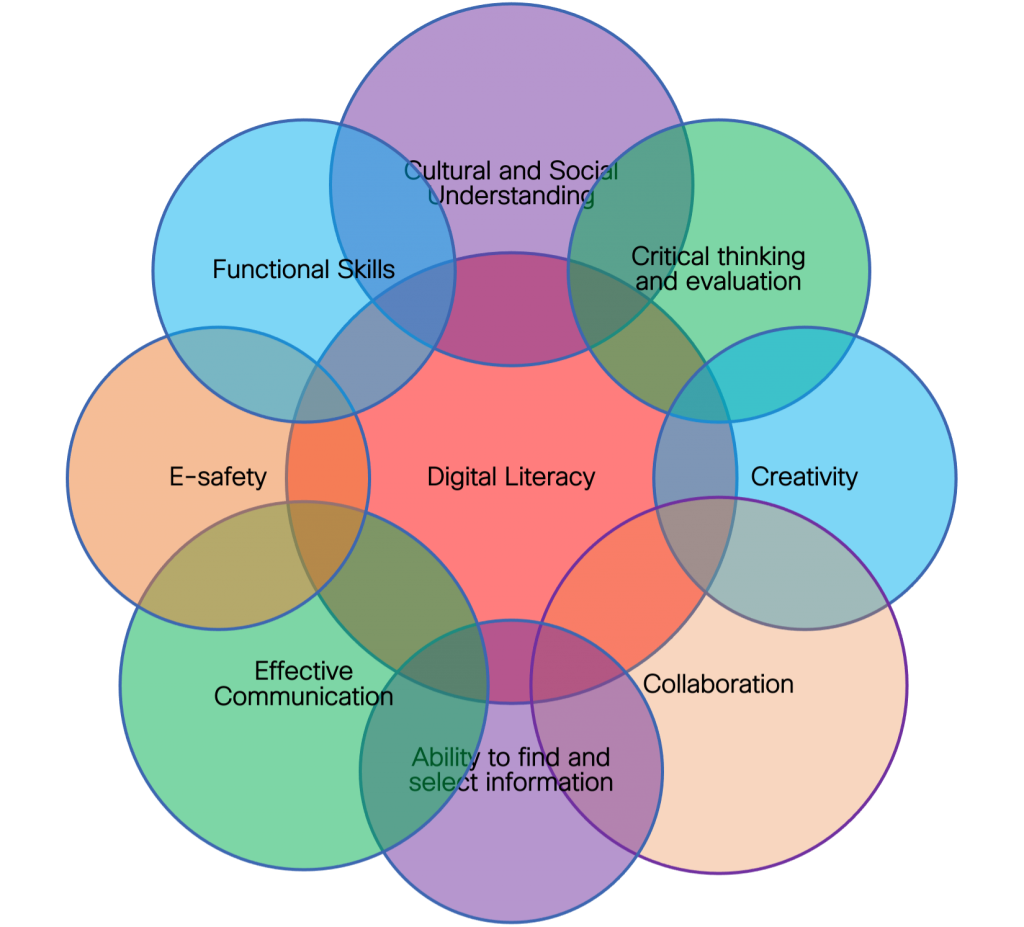
As part of the Digital Innovation Hub at La Trobe University, Cisco’s Innovation Central Melbourne set out to define digital literacy for healthcare. With this initiative, Cisco and La Trobe University examined how the healthcare workforce can become more digitally driven, with data and technology creating valuable insights, enhanced clinical efficiencies and knowledge-flow-to-value for patients. Digital literacy is using technology and tools to lead to more efficient use of staff, better care coordination, improved patient experience and better enterprise performance against key performance indicators (KPIs), such as: bed turnover rate, average length of stay, occupancy rate, and patient satisfaction. The big picture is not just about technology. Digital culture is also focused on social and cultural issues, communication, and collaboration.
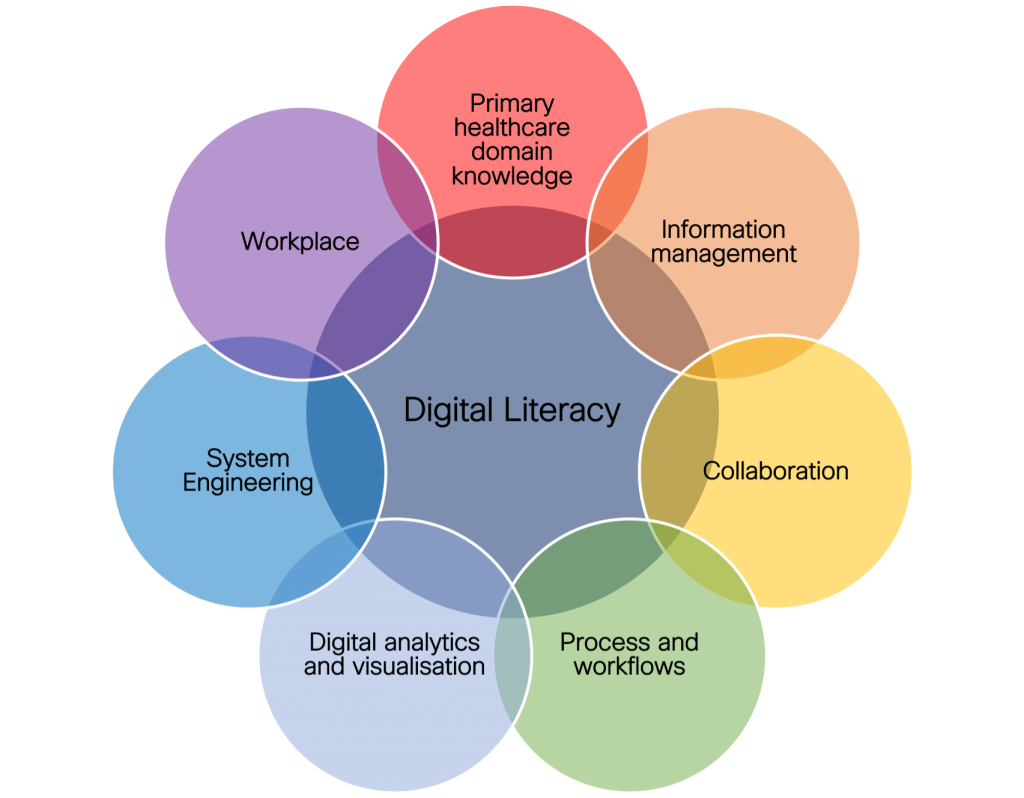
The Potential of Digital Culture in Healthcare This figure shows a bespoke group of knowledge domains needed to establish a digital culture and create patient value from data and insights. Taken as a holistic approach, the combination of knowledge domains, key technologies, and core learning objectives add up to a requirement for hands-on learning, and digital and data literacy.
Adjustments to learning content for different levels of workers and leadership would allow this map to be applied across any organization, at any level, and for executives to learn-by-doing along with their workforce. Implementing a Digital Culture Within Your Workforce Through this initiative, one consistent theme we recognized is that implementing services for digital devices and data can be a challenge for healthcare organizations. For healthcare organizations looking at driving a digital culture in the workplace, one of the most costly and dynamic challenges is the management of people and their devices. Here are five things to consider when optimizing operations with a focus on digital:
To create a true digital culture within your healthcare workforce, you need to consider how to:
At Cisco’s Innovation Central Melbourne, we have programs like MasterTech, where leaders collaborate to create and pilot technology solutions to take back to their workplaces. We welcome the opportunity to partner with your healthcare organization to help you drive a culture of digital literacy. To learn more about Cisco’s Innovation Central Melbourne and how we can best support you, please contact me directly ([email protected]). Cisco’s Innovation Central Melbourne is part of the National Industry Innovation Network. from https://ift.tt/oa5rGfZ Check out http://felpec.wordpress.com The future of healthcare is being driven by innovation and digital transformation, with a heightened focus on open-standards interoperability and distributed ecosystems. While the acceleration of digital technologies, IoT, the Internet of Medical Things (IoMT) and medical device utilization has been beneficial in driving more informed care delivery and greater access to care, the introduction of more devices on the network creates increased risk across the threat landscape. Keeping up with cybersecurity threats has always been a challenge, but today the speed at which new threats are introduced is astounding. When it comes to security in healthcare, it’s clear that uncertainty has become the new normal. Many organizations are not sure how to identify and manage digital risks in the ever-changing threat landscape, and their current risk management strategies just can’t keep up. We encourage you to explore our new thought leadership paper titled “Cybersecurity threats are top of mind for healthcare CIOs and CISOs,” where we explore:
from https://ift.tt/7omC6WA Check out http://felpec.wordpress.com After welcoming a new baby, the last thing that a parent wants to do is to leave the baby in the care of someone else. But that’s often the situation for parents and families of newborns in the Neonatal Intensive Care Unit (NICU). Due to the nature of care and the NICU environment, parents and family members cannot always be with the baby 24/7. They may even miss critical milestones or updates if they need to step away from the NICU for work, to care for other children or even to get some much-needed rest. Today at IWK Health in Halifax, Canada, that’s not the case. IWK’s Chez NICU Home program provides families with online education, resources, and virtual connections to help them become more active participants in the care of their baby while in the NICU. Chez NICU Home includes a web-delivered application created by the IWK that provides evidence-based education and resources for families with the ability to track their infant’s progress. From daily care activities, feeding and nursing, to the discharge process and understanding common NICU conditions, Chez NICU Home provides families with the information they need at anytime, anywhere. 97% of families that participated in the Chez NICU Home application agreed that the resources were extremely beneficial during an otherwise stressful time. Each NICU room is also equipped with a high-quality Webex video device and collaboration technology that connects families to appointments with healthcare providers and local health professionals, or to family members who are unable to be there in person. For example, if spouses need to care for other children out of town, they can virtually participate in clinical rounds via Webex to get the latest update on the baby’s progress. Leveraging Cisco technology to provide critical support and virtual connections has helped more than 450 families thrive during their stay in the NICU at IWK Health. Chez NICU Home was a collaboration across IWK Health that included Innovation Services, a team of researchers, clinicians, and IT, in partnership with Cisco Canada and OnX. It was developed with support and financial contribution from the Government of Canada through the Atlantic Canada Opportunities Agency (ACOA) and the IWK Foundation. from https://ift.tt/xsfycUG Check out http://felpec.wordpress.com This post is authored by guest contributor Professor Vishaal Kishore, the Executive Chair of the Cisco-RMIT Health Transformation Lab The recent report of the Australian Royal Commission into Aged Care Quality and Safety tells us two critical things. First – something systemic is going on in aged care: the elements of the system are not working together to produce optimal outcomes. Second – the issue is one of respect: our system is not treating individuals the way that they ought to be treated. Our challenge is to find a way to make the Australian aged care system simultaneously more connected, and more compassionate. And this is where technology has a crucial role to play – but the role is a complex one. Done right, technology can be core to making our system more respectful. Done poorly, technology can merely contribute to making a disrespectful system more efficient at being disrespectful. At the Health Transformation Lab, we – along with Cisco – set out to explore the profound role that technology can play in reorienting our aged care systems around connection and respect. But those of us who work in innovation in the care economy know that words are not enough – so we set out not just to write about why technology can transform aged care, but also to demonstrate how. The end result is something of which we all are deeply proud – in a few short months RMIT and Cisco had been able to demonstrate how technology could be used to improve the experience of people in aged care and also free up much needed time for staff to focus on their core role: delivering care. Perhaps most excitingly, these technologies all exist right now – our task is just to arrange them and deploy them in new and exciting ways. In the coming months, the Health Transformation Lab is looking to work with industry partners, providers and others interested in doing something meaningful to improve the lives of people receiving aged care services in a multitude of settings. Based on our initial demonstrations I am confident that government and the sector broadly will start to understand that technology is not something to be balanced against ‘human-to-human’ care, but rather the very thing that enables it. To learn more about how the collaboration with Cisco combines research and technology to address key recommendations, read our report on Transforming Aged Care. from https://ift.tt/a4Uiest Check out http://felpec.wordpress.com Today’s healthcare environment looks very different than it did just a few years ago. Healthcare is no longer delivered exclusively inside the four walls of a care setting, which enables better access for patients and a more efficient experience for clinicians and administrative staff. Technology can be used to more easily schedule and triage patients, collaborate amongst clinicians and care providers both onsite and off, and follow up virtually with care at home. A flexible work environment allows often stressed and burnt-out clinicians to take much-needed physical and mental breaks, which is critically important in a field that is losing talent and already has a global shortage of skilled healthcare workers (the United States is projecting a shortfall of 124,000 skilled healthcare workers in the next twelve years). Recently, we commissioned IDC to explore workplace transformation in healthcare and the ways that healthcare organizations are taking a digital-first approach to care delivery. The result is a new Industry Spotlight paper titled, “Workplace Transformation in Healthcare: The Time is Now.” The spotlight uncovered some interesting statistics about the benefits healthcare providers reported after implementing a more flexible work model. When asked in IDC’s Hybrid Work Maturity Study what percentage improvement their organization experienced in 2021 because of investments in work transformation, healthcare providers reported having achieved a marked improvement in employee experience (30%), expanding the talent pool beyond existing geographical constraints (28%), attracting top talent (29%), and better employee retention (29%). Out of necessity, hybrid work was adopted during the pandemic across all industries. And while healthcare has reverted to a more traditional care setting, elements of a hybrid model still exist because patients and providers demand it. What we’re starting to see now is the next wave of innovation in healthcare. One that moves beyond virtual care, digital front door and clinical communications to address the healthcare facilities themselves. While the technology we’ve adopted in the past few years that enables better communication and virtual care is still critical, healthcare organizations are now also investing in smart and sustainable hospital facilities to address Environmental, Social and Governance goals (ESG) and differentiate amongst competition. With smart and sustainable hospital facilities, healthcare organizations can reduce energy consumption, water usage and waste, enable greater automation and security for systems across the facility, and address the future of work with smart, intuitive, and flexible spaces. Ready to learn more about workplace transformation in healthcare and the numerous benefits to healthcare staff and their patients? We encourage you to read IDC’s spotlight on the future of workplace transformation in healthcare (Doc #US49224922, June 2022), and join the conversation by sharing your thoughts in the comments below. from https://ift.tt/ac7ErTn Check out http://felpec.wordpress.com Virtual care comes in many forms and the term covers a multitude of use cases and workflows. We find that providers can deliver better remote care, at lower cost, when they standardize on a virtual care platform with the ability to support all core use cases. At Cisco, we’ve taken a full-stack platform approach that leverages the power of our Webex service, together with software and hardware deployed across the cloud and the premise, to deliver the best possible end-user experience and scale across the many use cases of virtual care. So, what are some of the use cases for virtual care and how can technology drive adoption and scale? Reducing the need for meetingsWith asynchronous video, we give administrators and clinicians the ability to easily record and publish short video messages to a group of stakeholders. Video makes the message more personal than a simple email, is available for consumption at the recipient’s convenience and reduces the need for yet another meeting. Facilitating effective hybrid meetings and trainingFor team meetings or training sessions, the new Webex service has been re-designed to drive engagement and inclusivity. We want every meeting participant to contribute their ideas to the team. The right video device in each workspace simplifies the meeting experience for clinicians and administrators and allows groups of people in the hospital to be together in a physical meeting space while still connecting and collaborating with remote team members. Managing community outreachWebex Events is designed to provide end-to-end management of larger scale events. For example, community engagement or fundraising. By supporting all the different work streams that are needed to pull off a successful large-scale event, Webex Events can be fully virtual, physical or a mix of both. World-class remote patient consultsFor telehealth consultations, our team of healthcare experts have purpose-built Webex Instant Connect. This sits on top of the Webex platform and delivers on four key elements to virtual care at scale: Integration in clinician workflow through Electronic Health Records (EHR) systems, easy access for all patients, security and being manageable at scale. To learn more about how to specifically drive telehealth adoption within your healthcare organization, we recommend reading one of our past blog posts on the subject. This capability is also helping drive healthcare equity in rural areas of the country. Exam rooms are equipped with fit-for-purpose video devices. The healthcare system schedules a consult for the remote patient with a clinician who is physically in one of their larger hospitals. The clinician uses Webex Instant Connect to schedule and start the virtual session. The medical assistant uses the video device in the remote clinic to bring the patient and doctor together over the virtual call. The quality of that call is high because the institution controls network bandwidth in the clinic and the video device is built around state-of-the-art components. |





 RSS Feed
RSS Feed
